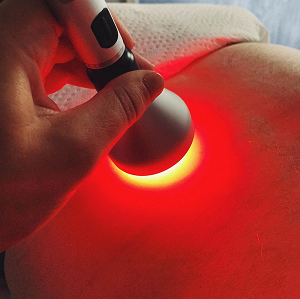
The Growing Science of Photobiomodulation: A Field on the Rise
Photobiomodulation therapy stands at a fascinating crossroads: a modality with compelling biological mechanisms, an expanding body of clinical evidence, and a research community whose enthusiasm far outpaces its funding. Understanding where PBM has been, and where it is going, helps explain why so many clinicians and researchers are betting on its future.
The science itself is elegant. When specific wavelengths of red and near-infrared light interact with mitochondrial chromophores, they trigger a cascade of downstream effects - increased ATP production, reduced oxidative stress, modulated inflammation, and enhanced tissue repair. These are not speculative claims; they are reproducible findings documented across thousands of peer-reviewed studies spanning cell cultures, animal models, and human clinical trials.
Yet funding has remained a persistent obstacle. PBM doesn't fit neatly into the pharmaceutical paradigm that dominates research grant structures. There is no patentable molecule, no billion-dollar drug approval pathway to attract venture capital, and no single corporate benefactor with the incentive to fund large randomized controlled trials. Government agencies like the NIH have historically underfunded light-based therapies, leaving much of the research to academic enthusiasts and international investigators working with modest resources.
Despite these headwinds, the trajectory is unmistakably upward. In 2017, fewer than 4,000 PBM papers had been indexed on PubMed. Today that number has grown exponentially, with studies now conducted in over 70 countries exploring applications from neuropathic pain and wound healing to neurological conditions and cancer care. The 2016 addition of "photobiomodulation therapy" as an official MeSH term was a pivotal moment — legitimizing the field's vocabulary and making its literature far more discoverable.
The momentum is real. As the published evidence compounds, so does credibility - and with credibility comes the funding, the clinical adoption, and the patient outcomes this field has always promised.
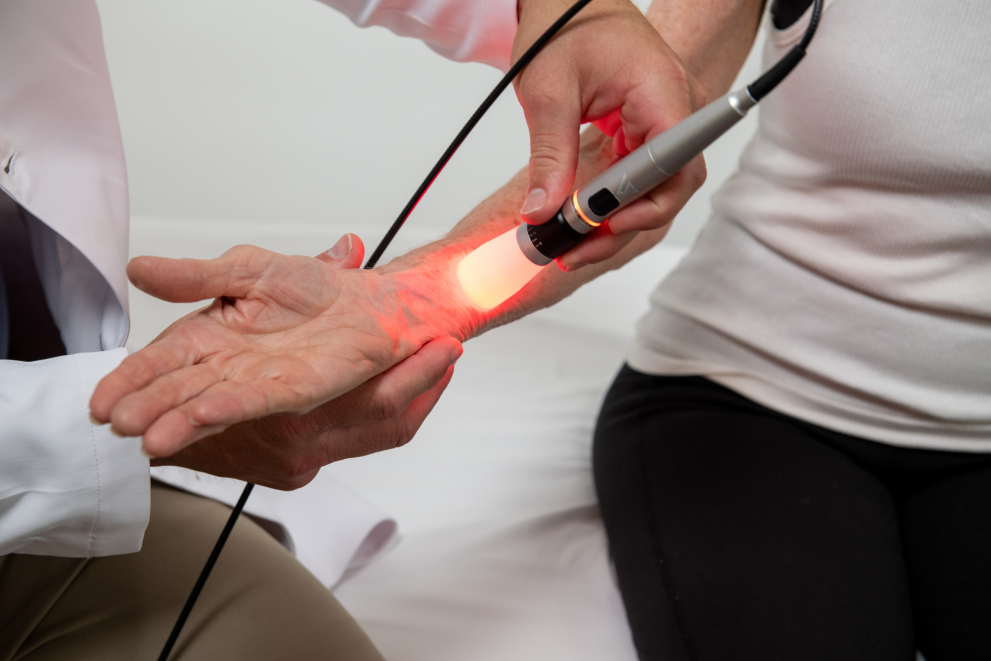
The Therapeutic Effects of Red and Near-Infrared Light
Red light and near-infrared irradiation produce measurable changes locally in cells/tissues/organs. This form of light therapy is called photobiomodulation (PBM).
Animal studies show that photobiomodulation therapy could be beneficial for over 100 different diseases. Evidence from human studies is also emerging in a fast pace.
Over 3800 photobiomodulation papers have been published in PubMed-indexed journals, over 120 of which have a good impact factor (> 3.0). Research has been conducted in at least 71 different countries.
The mechanistic basis for photobiomodulation therapy of neuropathic pain by near infrared laser light.
Conclusion: These in vitro and in vivo studies indicate that treatment with an irradiance/fluence rate at 270 mW/cm2 or higher at the level of the nerve can rapidly block pain transmission. A combination therapy is proposed to treat neuropathic pain with initial high irradiance/fluence rates for fast pain relief, followed by low irradiance/fluence rates for prolonged pain relief by altering chronic inflammation.

“Therapy lasers have been an exciting addition to the health care treatment arsenal. The development of Class IV therapy lasers represents the next generation of light therapy. By maximizing the primary effects, Class IV therapy lasers are able to induce extremely rapid clinical responses. Progressive health care providers wanting to offer the latest technology to their clientele should investigate Class IV therapy lasers.”
— Dr. Julian Vickers (deceased)
Note from Dr. Phil
Dr. Julian was taken away from us too soon. He passed away in 2009, shortly after he and I authored this article on Class 4 Laser Therapy. He was a good man. I think of him often, and I look forward to seeing him again on the other side.